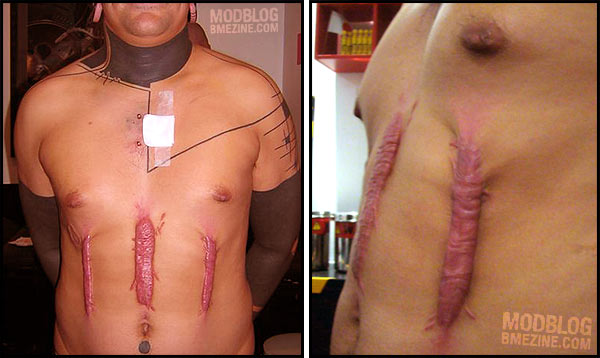
Keloid Scarring
Causes of keloid scars
From Jerry Kennard
Keloid scars are defined as an abnormal scar that grows beyond the boundary of the original site of a skin injury. It is a raised and ill defined growth of skin in the area of damaged skin. Although anyone can form a keloid scar some ethnic groups are at more risk of developing them.You are 16% more susceptable if you are African-American or Hispanic. Keloid scars are seen 15 times more in highly pigmented ethnic groups rather than Caucasians.
Parts of the body susceptible to keloids
Some areas of the body do seem more susceptible, the deltoid region of the upper arm, the upper back, and the sternum. The earlobes and the back of the neck are common sites.
Causes of keloid scars
It is not fully understood why or how keloid scars occur. Skin trauma appears to be the most common factor although they can form and there seems no apparent causation. Skin and/or muscle tension seem to contribute to keloid formation and this is demonstrated by the most common sites of their formation (the upper arm and back). However if that was the full story you would expect that other sites, such as the palm of the hand or the soles of the feet to be just as vulnerable, but this is not the case. Infection at a wound site, repeated trauma to the same area, skin tension or a foreign body in a wound can also be factors.
There does appears to be a genetic component to keloid scarring. It is known that if someone in your family has keloids then you are at increased risk.
Other theories for the causes of keloid scarring include a deficiency or an excess in melanocyte hormone (MSH), decreased percentages of mature collagen and increased soluble collagen, or that very small blood vessels get blocked and the resulting lack of oxygen contribute to keloid formation.
Whilst the lack of a clear cut theory does demonstrate the lack of understanding of the condition, some work is being done to find the cause. Finding out the exact cause will hopefully mean better preventative medicine and more effective treatments in the future, but there are many problems with adequate follow up of people with the condition, lack of a clear cut-off from treatment and just too few studies in general hampering the search for a cure.
Can you prevent keloid scars?
The fact is that there may be little you can do if you are unfortunate enough to have the sort of skin that reacts by forming keloid scarring. You can assist the healing process by keeping any wounds clean, that may help. If you know you are susceptible because of previous experience or a family connection then you can avoid taking extra risks. Do not have piercing or tattoos and make sure you tell your doctor if you are going to have surgery.
There is a high rate of recurrence - up to 50%. Some doctors say that all highly pigmented people should avoid tattoos and piercing to be on the safe side.
Treatment for keloid scars
There are 3 treatment options for keloid scars:
surgical removal
non-surgical interventions
combination treatments.
I will briefly discuss each one.
Surgical treatment of keloid scars
This is the most effective and the least complex of the available forms of treatment, the recurrence rate however is thought to be about 50%.
Lasers have been tried as an alternative to knife surgery but so far the outcomes are no better.
Non surgical treatments for keloid scars
Interferon therapy (drugs acting on the immune system), has been reported as effective in reducing keloid scarring however it does have significant side effects. Examples are toxicity, flu like symptoms, depression, nausea and vomiting. Prolonged compression of scar tissue can theoretically soften and break up keloid scars, however the practicality of this option depends on the location of the keloid. Other non-surgical interventions that are currently being tried with varying results include antihistamines, vitamins, nitrogen mustard, Verapamil, retinoic acids.
Combined treatments for keloid scarring
One option involves surgical removal of scar tissue in combination with a couple of steroid injections -one at the time of the surgery and the second injection about 3 to 4 weeks later. However, this type of treatment is variously reported as having between a 50% to 70% rate of recurrence.
Another option combines surgery with external type radiotherapy. Radiation has the effect of interfering with skin growth (fibroblasts) and collagen production. Research varies on which type of combination therapy is the more effective. Both radiotherapy and steroid drugs have side effects so you need to discuss with your doctor the most effective. It may be worth getting a second opinion before proceeding with either treatment.